Article and Study Summary:
Community-based antiretroviral therapy versus standard clinic-based services for HIV in South Africa and Uganda (DO ART): a randomised trial.
Published in:
Lancet Glob Health. 2020;8(10):e1305-e1315. https://doi.org/10.1016/S2214-109X(20)30313-2
Authors:
Barnabas RV, Szpiro AA, van Rooyen H, et al for the Delivery Optimization of Antiretroviral Therapy (DO ART) Study Team
Summary:
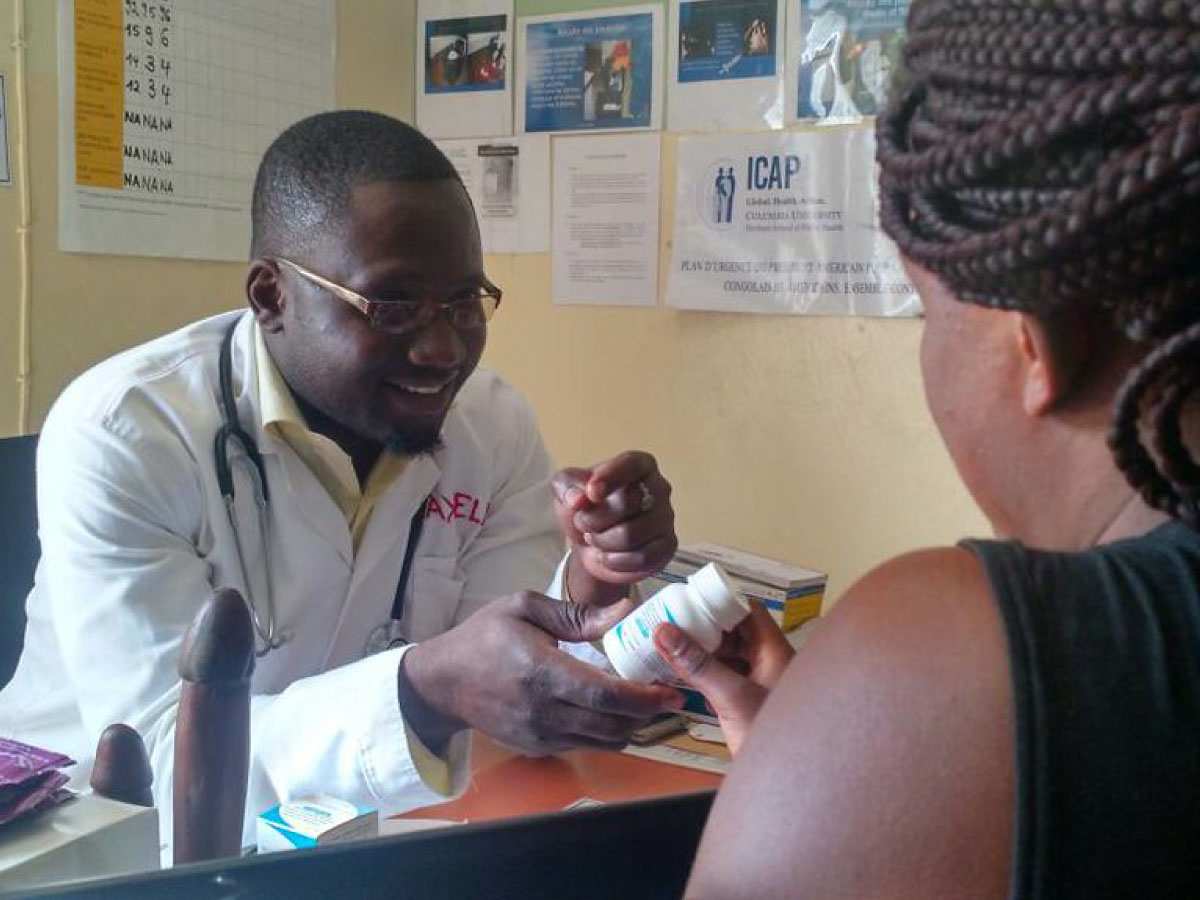
The Delivery Optimization of Antiretroviral Therapy (DO ART) study was a multicenter, randomized trial that compared antiretroviral therapy (ART) service delivery models for people living with HIV (PLHIV) in South Africa and Uganda. Adult PLHIV who were clinically stable and not on ART, were randomized either a community-based ART group, hybrid group or standard clinical care group. The community-based ART group received all ART-related services in the community, including same-day ART initiation, clinical monitoring using a mobile van, and ART refills. The hybrid group were referred to a clinic to initiate ART, after which they receive follow-up services in the community identical to the community-based group. The clinic group were referred to a clinic to receive standard ART services. The primary outcome of interest was proportion of participants achieving viral suppression after 12 months. The results showed that the community-based group had superior viral suppression to the clinic group, and the hybrid group had non-inferior viral suppression compare to the clinic group. Improvement in viral suppression with community-based services was especially notable in men, and it helped close the gender gap in viral suppression compared to women. These findings suggest that an ART service delivery model that is entirely community-based could help improve treatment outcomes, especially in men.
Discussion Questions:
- How could the findings in this study impact policy where you work?
- How could elements of this intervention be applied in programs you work with? Do you have any experiences to share?
Please share your thoughts and experiences with us in the comments section below.
Full Synopsis:
PDF version available in English, French and Portuguese.
Study Summary
The DISCOVER study is a randomized, double-blind, multi-center, non-inferiority trial that compared the efficacy and safety of pre-exposure prophylaxis (PrEP) with emtricitabine and tenofovir alafenamide (F/TAF) versus emtricitabine and tenofovir disoproxil fumarate (F/TDF) for the prevention of HIV among cisgender men who have sex with men (MSM) and transgender women (TGW) who have sex with men.
Study Setting
- Ninety-four community, public health, and hospital-associated clinics, located in Europe (Austria, Denmark, France, Germany, Ireland, Italy, Netherlands, Spain, and the United Kingdom) and North America (Canada and the United States of America) where HIV prevalence and/or incidence was high among cisgender MSM and TGW who have sex with men.
Methods
- The study enrolled HIV-negative, adult, cisgender MSM and TGW who have sex with men, with a high risk of acquiring HIV based on either self-reported condomless anal sex with >2 partners in the previous 12 weeks or having had syphilis, rectal gonorrhea, or rectal chlamydia in the previous 24 weeks.
- Individuals with the following conditions were excluded: a suspected or known active serious infection; acute hepatitis A, B, or C, or chronic hepatitis B infection; history of osteoporosis or fragility fractures; or impaired renal function, as defined by an estimated glomerular filtration rate (eGFR) by the Cockcroft-Gault formula of <60 mL/minute.
- Participants were randomly assigned (1:1) to receive once daily tablets of either emtricitabine 200 mg and tenofovir alafenamide 25 mg (F/TAF group) or emtricitabine 200 mg and tenofovir disoproxil fumarate 300 mg (F/TDF group). Participants in both groups also received placebo tablets that were identical in appearance to the alternative study drug, therefore all participants took two pills daily.
- After enrollment, study visits were at weeks 4 and 12, and then every 12 weeks. At each visit participants underwent clinical evaluation, adverse event evaluation, HIV testing with a rapid third-generation antibody test or fourth-generation antigen-antibody test, and laboratory testing for sexually transmitted infections (STIs).
- Sites provided local standard-of-care risk reduction counselling, adherence counselling, condoms and lubricant. Treatment for STIs and HIV post-exposure prophylaxis were offered as per local guidelines.
- Adherence was assessed at follow-up visits by use of a computer-assisted self-interview for self-reporting and by pill count. In a random subset of 10% of participants, adherence was evaluated further by quantifying tenofovir diphosphate concentrations in dried blood spots (DBS).
- At baseline and every 48 weeks, dual energy x-ray absorptiometry (DXA) scans of the hip and lumbar spine were done in a subset of 383 participants.
- The primary efficacy outcome was incident HIV infection, which was evaluated when all participants had been followed for a minimum of 48 weeks, and at least 50% had been followed for 96 weeks.
- Pre-specified secondary outcomes included: changes in renal biomarkers and bone mineral density at 48 weeks; treatment-emergent adverse events; changes in weight; and adherence by self-reporting, pill counts, and DBS testing.
- The primary outcome was evaluated in all participants who received at least one dose of the study drug and had at least one follow-up HIV test. The safety analysis population included all participants who received at least one dose of the study drug.
Study Population and Follow-up
- Between September 2016 and June 2017, 5,857 individuals were screened, and 5,399 were randomly assigned to either the F/TAF group (n=2,700) or the F/TDF group (n=2,699).
- The analysis set for the primary endpoint consisted of 5,335 participants (2670 in the F/TAF group and 2,665 in the F/TDF group). The safety analysis population consisted of 5387 participants (2694 in the F/TAF group and 2,693 in the F/TDF group).
- The median age of participants was 34 years (interquartile range [IQR] 28-43). The majority of the participants were white (84%), with 24% identifying as of Hispanic or Latinx ethnicity and 9% identifying as black.
- Most participants (91%) self-identified as gay, 1% were TGW and 23% reported ever using TDF for PrEP.
Primary Outcome
- After 8,756 person-years of follow-up, 22 participants were diagnosed with HIV, seven in the F/TAF group (0.16 infections per 100 person-years, 95% confidence interval (CI) 0.06–0.33) and 15 in the F/TDF group (0.34 infections per 100 person-years, 95% CI 0.19-0.56).
- Of those diagnosed with HIV, one participant in the F/TAF group and four in the F/TDF group were suspected to have acquired HIV before enrollment.
- F/TAF was non-inferior to F/TDF for the prevention of HIV, as the upper limit of the 95% CI of the incidence rate ratio (IRR) was less than the pre-specified non-inferiority margin of 1.62 (IRR 0.47, 95% CI 0.19-1.15).
Secondary Outcomes
- F/TAF was superior to F/TDF after 48 weeks in all pre-specified renal biomarker and bone mineral density safety endpoints.
- In the DXA subset, a significant difference in change from baseline was observed between the two groups in hip bone mineral density (p<0.0001) and spine bone mineral density (p<0.0001), with a decrease in bone density in the F/TDF group and stable or increased bone density in the F/TAF group.
- Participants in the F/TAF group had a median decrease in serum creatinine (Cr) of 0.88 μmol/L and a median increase in eGFR of 1.8 mL/min from baseline, whereas participants in the F/TDF group had an increase in median creatinine of 0.88 μmol/L and a decrease in eGFR of 2.3 mL/min (p<0.0001 for both).
- Participants in both groups had similar numbers of adverse events, with gastrointestinal symptoms most commonly attributed to the study drugs, including diarrhea (5% of participants in the F/TAF group and 6% in the F/TDF group) and nausea (4% in the F/TAF group and 5% in the F/TDF group) within the first four weeks.
- Incidence of adverse events that led to premature discontinuation of the study drug was similarly low between the two groups (1% of F/TAF group and 2% of F/TDF group).
- Renal adverse events occurred in 10% of participants in both the F/TAF and F/TDF groups, respectively, with events that were considered related to the study drug occurring in 0.5% of participants in the F/TAF group and 1% in the F/TDF group.
- Participants in the F/TDF group had a mean change in weight of –0.1 kg, whereas those in the F/TAF group had a mean increase in weight of 1.1 kg at week 48 (p<0.0001).
- There were no differences in adherence between the two groups by self-report, pill count, and DBS analysis.
- Between 96-98% of participants reported taking the study drug more than 80% of the time across all study visits.
- Median pill count adherence was 98% (IQR 93.4-99.8) in the F/TAF group and 98% (93.5-99.9) in the F/TDF group.
- DBS analysis in a subset of participants showed that 84-96% had tenofovir diphosphate concentrations consistent with taking four or more tablets per week.
Critical Analysis
The randomized, double-blind, multi-center, non-inferiority DISCOVER trial of PrEP found that daily F/TAF has non-inferior efficacy compared to daily F/TDF for HIV prevention in at-risk cisgender MSM and TGW who have sex with men in high-income settings. F/TAF also had more favorable effects on bone mineral density and biomarkers of renal safety compared to F/TDF, however both regimens were safe and well tolerated.
The following points should be considered when interpreting the study findings:
- Excluding the five participants with suspected baseline HIV infections, the majority (88%) of the remaining 17 participants who were diagnosed with HIV during follow-up had low (average of <2 doses per week) or undetectable tenofovir diphosphate concentrations in DBS on the day of HIV diagnosis. This suggests adherence remains essential for PrEP drugs to be efficacious in preventing HIV infection.
- The HIV incident rate in the study population was lower than expected, however there was still evidence of risky sexual behavior as ≥10% of adverse events were bacterial STIs and STI rates were similar between the two groups.
- A very small number of TGW were included in the study, therefore it was not possible to assess any potential differences in outcomes between MSM and TGW.
- The study was not designed to evaluate the efficacy of F/TAF as PrEP for those who engage primarily in vaginal sex, therefore these results cannot be generalized to female populations engaged in receptive vaginal sex.
- Although F/TAF had more favorable biomarkers of renal safety and bone mineral density than F/TDF, there was no difference in clinically significant adverse events between the groups. It is possible, however, that clinically significant loss of renal function or bone mineral density could develop with more prolonged exposure to PrEP than was evaluated in this study.
Implications
The DISCOVER trial was a randomized, double-blind, multi-center study that demonstrated that daily oral F/TAF had non-inferior efficacy to F/TDF as PrEP to prevent HIV infection in MSM and TGW who have sex with men. As a result, F/TAF became the second PrEP regimen approved by the U.S. Food and Drug Administration in 20191. However, this approval remains limited to the populations studied and therefore does not include women engaged in receptive vaginal sex. While trials of F/TAF in other populations are planned, its use will likely be limited to high-income settings until it has a broader indication and a generic version is widely available. The approval of a regimen that requires less frequent renal monitoring can enable PrEP provision in a wider variety of non-clinical settings, which could increase access for those in need.
This article synopsis was written by Cassia Wells. Share your thoughts on this article or suggest an article for Journal Club by emailing her at caw2208@cumc.columbia.edu
References
- U.S. Food and Drug Administration, FDA News Release, “FDA approves second drug to prevent HIV infection as part of ongoing efforts to end the HIV epidemic”, October 3rd, 2019. Available at FDA.gov.