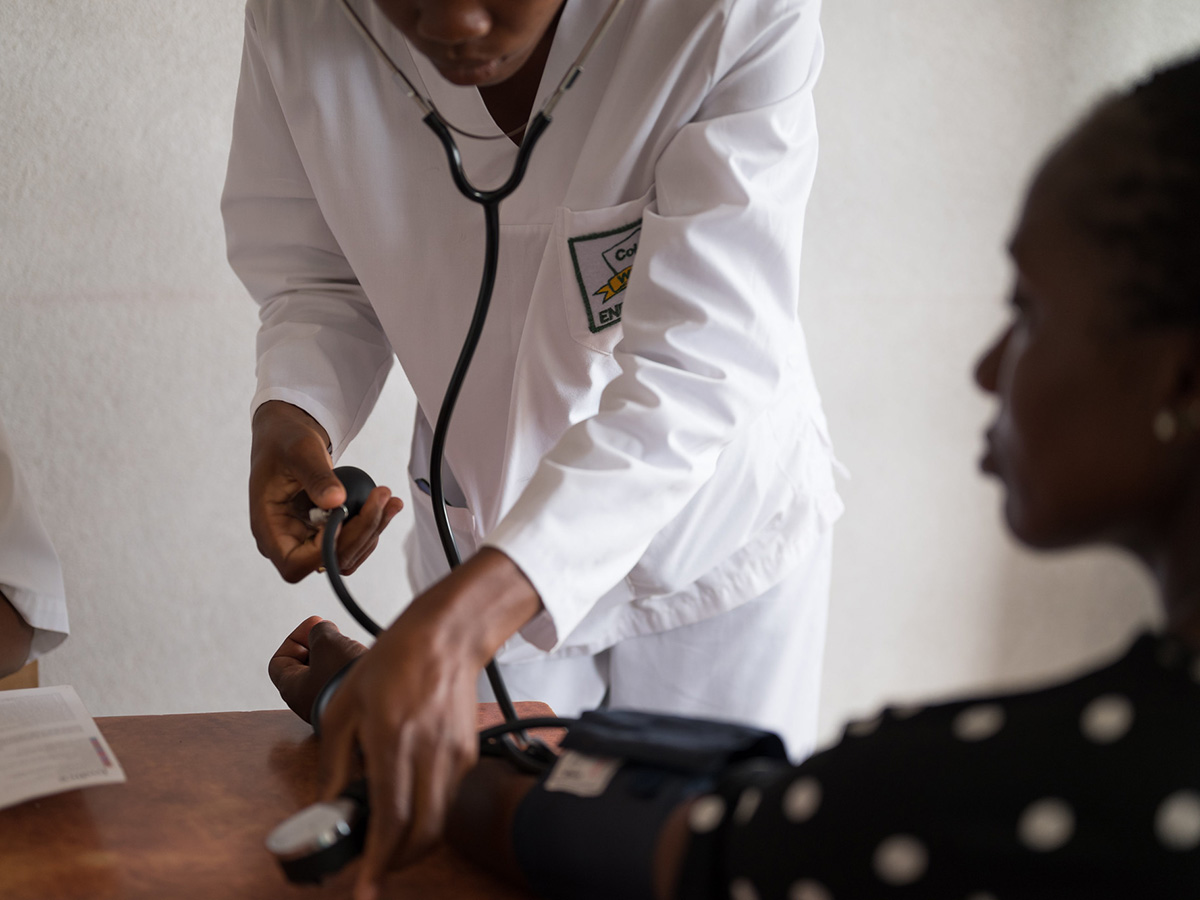
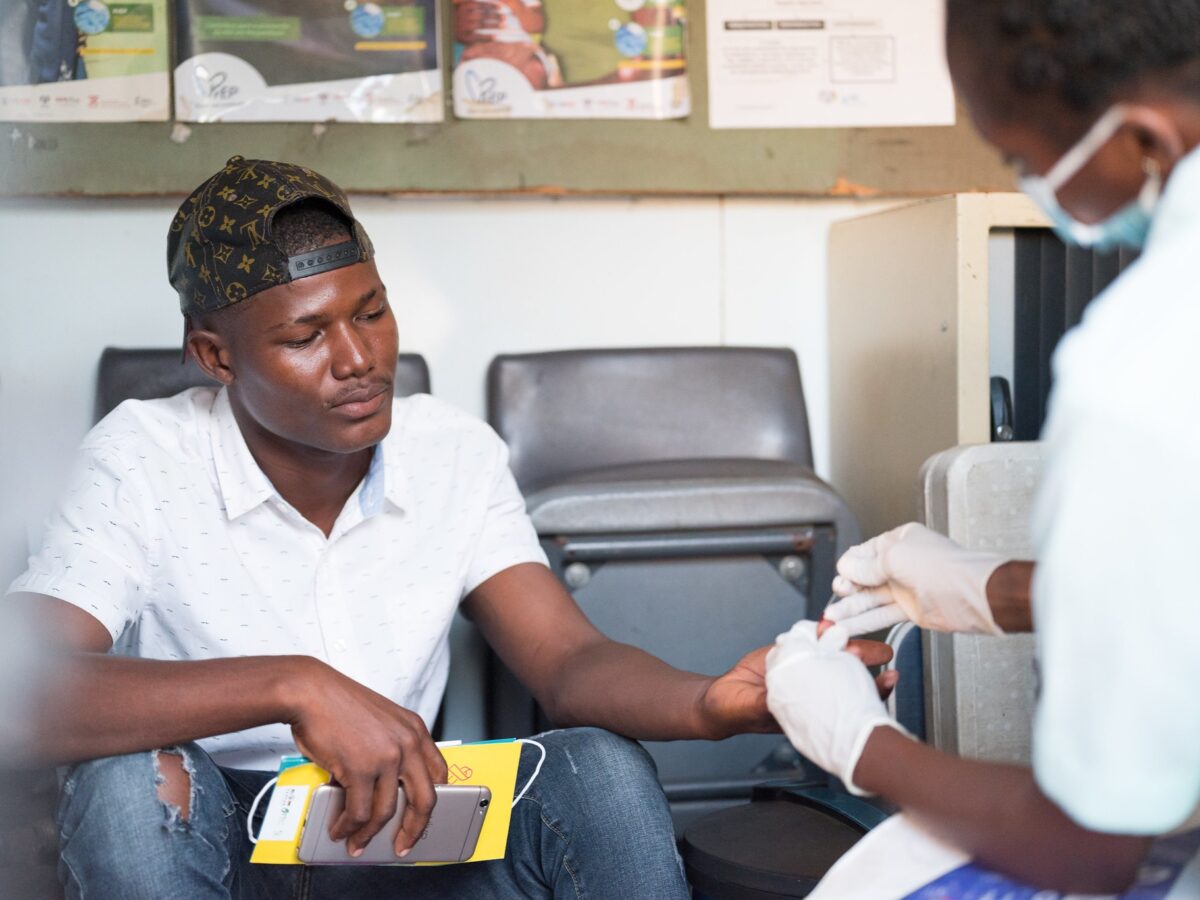
Tuberculosis is preventable, and yet, it afflicts 10 million people every year globally. The Kingdom of Lesotho accounts for the world’s highest incidence of tuberculosis (TB), with over half of cases co-infected with HIV. Children are especially vulnerable to developing severe forms of TB, but many go undiagnosed, lacking the lifesaving treatment they need.
The question that public health officials in Lesotho are asking is: What management strategies would be both effective and acceptable in addressing this pervasive disease?
The PREVENT study, which was led by ICAP at Columbia University, supported by the National Institute for Allergy & Infectious Diseases of the National Institutes of Health, and conducted in collaboration with the Lesotho Ministry of Health, demonstrated that delivery of a community-based intervention (CBI) significantly improved TB preventive treatment (TPT) initiation and completion among young child TB contacts in Lesotho and was highly acceptable to both health care providers and caregivers. CBI in the study involved a person-centered multicomponent strategy that holistically addressed the complex health care provider-, patient-, and caregiver-related barriers for the prevention of childhood TB.
PREVENT evaluated whether CBI could improve TB child contact management (CCM). CCM is a recognized contact tracing strategy to prevent TB disease in young children, but its implementation is suboptimal in high TB/HIV-burden settings. Ten health facilities within Berea District, Lesotho were randomly selected as either CBI sites or standard-of-care (SOC) sites. In addition to providing SOC, which included contact tracing, screening, and TPT provision, CBI comprised of nurse training and mentorship; health education and follow-up with caregivers of children who missed appointments or reported nonadherence by village health workers; real-time adherence support via weekly SMS messages; and multidisciplinary team meetings.

The PREVENT study demonstrated that a greater percentage of children initiated TPT in CBI sites than SOC sites, and, importantly, TPT completion was significantly higher in CBI sites compared to SOC sites at 82 percent versus 59 percent, respectively.
“The World Health Organization roadmap for childhood TB calls for an ‘integrated, family- and community-centered strategy’ to prevent and address TB, and CBI is responsive to that call by enabling health care providers to provide family-centered TB prevention services to children and their families,” said Yael Hirsch-Moverman, PhD, MPH, principal investigator of the study and senior technical advisor for ICAP’s Clinical and Training Unit. “This study shows us that delivery of multifaceted CBI is feasible, acceptable, and improved prevention of TB in a highly vulnerable population of young children who are susceptible to severe forms of TB.”
In Lesotho, 4 percent of TB cases are reported in children, which is low compared to similar settings – an indicator of under-detection or under-reporting. Caregivers involved in the study noted that CBI implementation was an important factor in addressing many of the barriers to TPT adherence they typically face. Medication reminders from village health workers, for example, as well as synchronized treatment and health facility visits facilitated adherence to medication and medical appointments.
Nurses and lead village health care workers were trained in how to implement CBI before the study launch and received refresher trainings and mentorship on-site from a study nurse mentor. These teams from CBI sites met quarterly to review data and intervention activities, identify challenges, and develop solutions. At CBI sites, nurses promoted TPT initiation, assessed TPT adherence and side effects, and encouraged follow-up with village health workers. Village health workers used a scripted, illustrated flipchart in health facilities and an illustrated brochure in the community to educate caregivers and children on the importance of TB prevention, TPT provision, and TPT adherence.

Brochures used by village health workers to deliver health education in the community.
Social support was noted as a valuable CBI site component among caregivers and health care providers. Village health care workers physically bringing caregivers medication when needed or providing information and advice pertaining to medication side effects closed gaps that often stall TPT completion.
“Beyond the assistance CBI gives caregivers and the patients themselves,” said Liamkatso Lebelo, a nurse mentor and an author of the study, “the CBI package is useful to health care workers as well, as it provided a systemic guidance on patient management from time of screening throughout the treatment phase and follow-up until treatment outcome using a flow chart and regular mentorship. This was seen to be very helpful compared to sites that implemented SOC, where the patient management was not well coordinated and there were a lot of missed steps and gaps in the whole management process, leading to poorer outcomes.”
“This study has important future implications for TB prevention in children in Lesotho and globally,” said Koen Frederix, a co-investigator and an author of the study. “Existing guidelines already recommend isoniazid prophylaxis for children, as safety and effectiveness have been proven. However, implementation is often poor because it may not be high on the priority list of health care workers and authorities. I hope this study will strengthen commitment and help to address the remaining barriers hindering implementation of isoniazid preventive therapy.”
With more than 200,000 children dying each year from TB, addressing the barriers to TB prevention and treatment for young people is urgent, especially amid the COVID-19 pandemic, which exacerbated already-constrained access to TB health services. In addition to the PREVENT study, ICAP recently completed the PROTECT study, which explored preferences regarding TPT regimens among children and adolescents in Eswatini, and is currently conducting the FIRST study, which is pilot-testing a family-centered flexible child TB contact management model in Eswatini.
“ICAP is committed to improving the health of children and adolescents in high TB/HIV burden settings,” said Andrea Howard, MD, MS, a co-investigator of the study and director of ICAP’s Clinical and Training Unit. “Through this body of research, we aim to improve implementation of evidence-based interventions to prevent TB in this vulnerable population.”
About ICAP
A major global health organization that has been improving public health in countries around the world for nearly two decades, ICAP works to transform the health of populations through innovation, science, and global collaboration. Based at Columbia Mailman School of Public Health, ICAP has projects in nearly 40 countries, working side-by-side with ministries of health and local governmental, non-governmental, academic, and community partners to confront some of the world’s greatest health challenges. Through evidence-informed programs, meaningful research, tailored technical assistance, effective training and education programs, and rigorous surveillance to measure and evaluate the impact of public health interventions, ICAP aims to realize a global vision of healthy people, empowered communities, and thriving societies.