Lete is a community counselor. She collaborates with one of ICAP at Columbia University’s mobile units, which provide comprehensive HIV and TB prevention, care, and treatment services integrated with general health services – including outpatient consultation and maternal and child health services – at the community level in Nampula, Mozambique. Supported by the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) through the Centers for Disease Control and Prevention (CDC), ICAP’s mobile units offer such services as HIV testing, pre-exposure prophylaxis (PrEP), condoms, anti-retroviral (ART) initiation and continuation, STI screening and treatment, psychosocial support, viral load testing, and TB prevention, free of charge.
Lete coordinates activities between the mobile unit and the community, engaging new people to take advantage of the health services offered by the clinic and presenting on such topics as the importance of taking PrEP or getting tested for HIV. As a woman living with HIV – and someone who also lost a parent to the virus – Lete builds trust with communities by using herself as an example of someone who successfully sought and maintained treatment for HIV, but she also understands some of the challenges people living with HIV face in accessing health services. Barriers such as stigma as well as long distances to health facilities impede people from initiating preventive health services as well as maintaining long-term, lifesaving treatment.
“This clinic is a safe space for people,” Lete said, “where they do not experience discrimination for accessing services like HIV testing or condoms.”
ICAP supports mobile units in 19 districts in Mozambique, serving general populations, key populations, adolescents and youth, and internally displaced people. Between October 2022 and March 2023, the mobile units served 23,951 people, of which 11,782 were tested for HIV, with 901 people identified as HIV-positive. Over the course of the year, a total of 1,252 people initiated ART.
Important components of the mobile units are the discretion of their health staff and their proximity to households, workplaces, or congregation areas. For example, ICAP’s mobile units provide health services at the office of the LAMBDA Association, an organization of Mozambicans who advocate for the rights of the LGBT community. Leaders within the group travel out into communities to increase awareness about the availability of the clinic’s services and ensure key populations are welcome.
“I came to the group in 2015,” said S, a member of LAMBDA who accesses ICAP’s mobile unit services. “There was an opportunity for me to become a community worker and I took it. It’s so rewarding to contribute to our community since many have not always had communities to go to.”

A LAMBDA member utilizing ICAP’s mobile unit for HIV testing learns he is HIV-negative.
In recent months, 124 communities – six on islands – have been reached by daytime mobile units, and 51 communities have been reached through evening mobile units. At the site Lete serves, the mobile unit parks at an evening “hotspot” often frequented by sex workers and their clients.
In addition to reaching remote communities and hotspots, the mobile units also provide health services for four private companies, three educational institutions, 17 prisons, three localities serving adolescents and youth, and one community with a high concentration of men.
“A crucial step to ending the HIV epidemic is making health services accessible,” said Eduarda Pimentel de Gusmao, MD, MPH, country director of ICAP in Mozambique. “Mobile units take away the guesswork. They meet communities where they are.”
On a recent evening following a common sudden Mozambiquan rain, people emerged from indoors to visit ICAP’s mobile unit parked at a hotspot in Nampula. As people began to socialize and dance to music crooning in the background, Lete met people where they were. From the door of the mobile unit, she surveyed the crowd and milled around to find people she wanted to follow-up with on how their treatment was going or to ask what services they may need. Lete, who is a mother of two, has worked as a community counselor for five years and has received extensive training on approaches to reaching hard-to-reach populations.
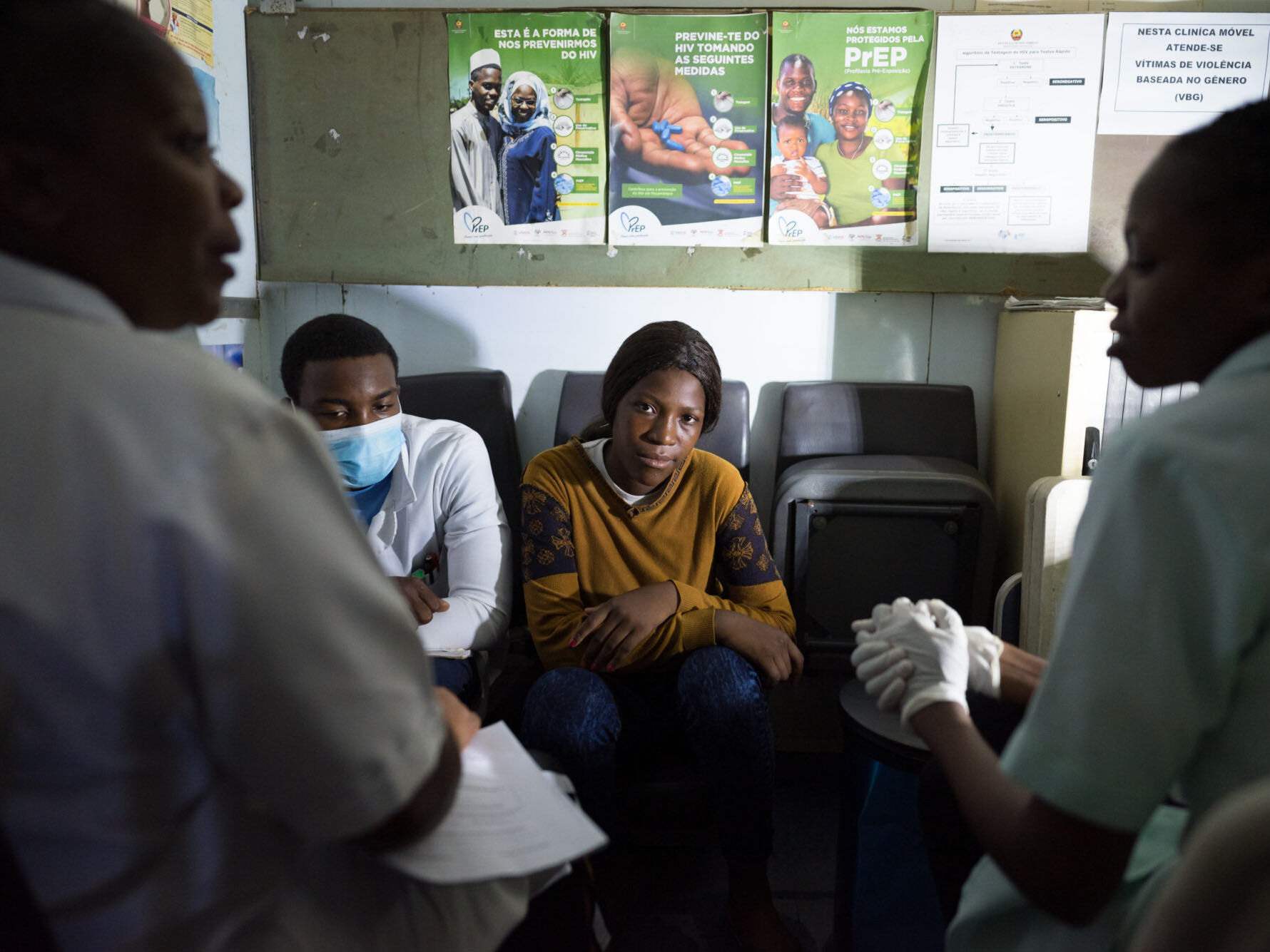
A woman gets tested for HIV in the mobile unit Lete serves.
“I was cautious when I came for my first test because my father died of HIV,” Lete said. “But now I look at anti-retroviral treatment as a second chance of life because I’ve seen what can happen when you don’t seek help.”
“I have a 12-year-old daughter who is HIV-negative, and she told me one day that she heard about HIV,” Lete added. “I’m very open with her. I used the opportunity to educate her by telling my story.”
Photos by Artur Francisco
About ICAP
A major global health organization that has been improving public health in countries around the world for nearly two decades, ICAP works to transform the health of populations through innovation, science, and global collaboration. Based at Columbia Mailman School of Public Health, ICAP has projects in more than 30 countries, working side-by-side with ministries of health and local governmental, non-governmental, academic, and community partners to confront some of the world’s greatest health challenges. Through evidence-informed programs, meaningful research, tailored technical assistance, effective training and education programs, and rigorous surveillance to measure and evaluate the impact of public health interventions, ICAP aims to realize a global vision of healthy people, empowered communities, and thriving societies.