In Bure, Ethiopia, malaria is a severe health threat. But for this town of 23,000 people in the country’s Amhara region, 250 miles northwest of the capital, distance was making the threat even more lethal.
More than two-thirds of Ethiopians live in malaria-prone areas and an estimated 2.7 million cases of malaria occur every year in the country. Although insecticide-treated nets and other prevention methods have made an impact, factors such as travel cost, distance to a health facility, and lack of resources available at the community level for reliable malaria testing have combined to prevent many people from getting the help they need.
But all that is changing for the people of Bure—and for many other communities across the nation.
“We used to have to refer patients with severe cases to Debremarkos Hospital, about 60 miles away,” said Alemtsehay Endeshaw, BSc, the laboratory expert at Bure Health Center. “But we now have the capacity for prompt confirmatory laboratory testing of malaria so we can confirm diagnosis before providing treatment.”
This expanded service, which is saving lives in Bure, comes from the health center’s partnership with ICAP in the Malaria Laboratory Diagnosis and Monitoring project, funded by the U.S. Agency for International Development (USAID) through the President’s Malaria Initiative (PMI).

Bure Health Center was one of 1,026 participating health facilities supported by the Ethiopian Federal Ministry of Health and PMI for rapid and improved malaria diagnosis and treatment as part of this project, which concluded in 2017. Building on nine years of success, the current Malaria Diagnosis and Treatment Activity began in 2018 and has so far been implemented in 680 participating health facilities spread across the 146 districts.
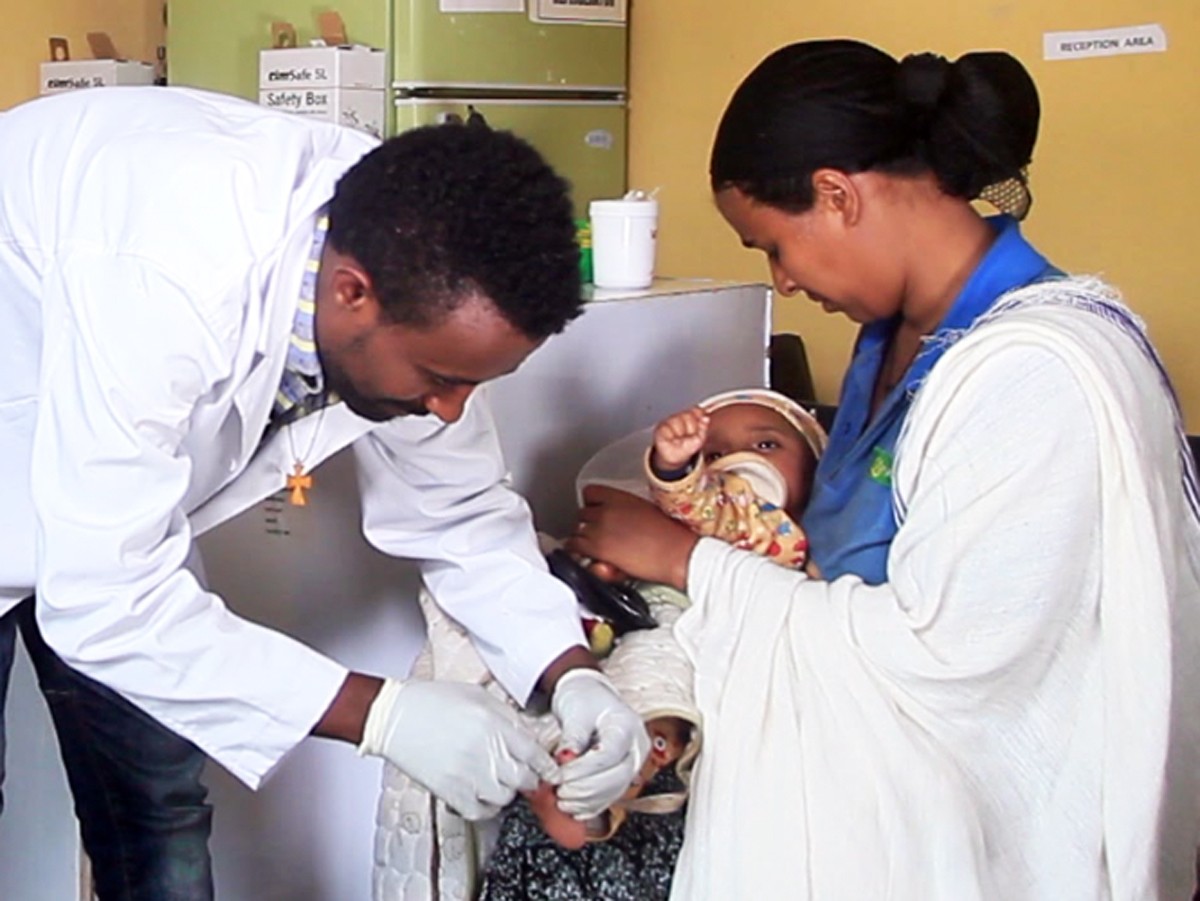
In Bure, Shitaye Abere knew exactly what to do when her child began showing signs of potential malaria. “My little child started to have fever and got sick overnight,” she said. “I suspected that might be malaria since our neighborhood is prone to malaria. Immediately I took him to the nearby Bure health center.”
At the health center, Shitaye was met by a health care worker who told her that her child would undergo a blood test to confirm whether his symptoms were indeed caused by malaria infection, and receive immediate treatment if indicated—all free of charge, since Ethiopia covers malaria diagnosis and treatment at all public health facilities as part of its national malaria control program.
“My guess came true: my child was diagnosed with recent malaria infection. I trusted the result because they did a blood test. After carefully looking after my child as advised by the health care worker and making the necessary treatment follow-up, my child has fully recovered and is now in good condition.”
Together with the Ministry of Health, ICAP has been working to make this outcome the norm across malaria-endemic regions of Ethiopia.

Microscopic diagnosis is the gold-standard for laboratory confirmation of malaria, but it requires very strong technical and institutional capacity, which facilities in semi-rural and rural parts of Ethiopia may not have.
Working with the Ministry of Health, ICAP assessed gaps in both the material and human resources needed to provide the highest standard of malaria testing and diagnosis at a community level, and equipped the laboratories at community health facilities with microscopes, centrifuges, reagents, consumables, and standardized support tools for improved malaria diagnostic service.
“The microscopes we have been provided are of the highest quality, which can even run with rechargeable batteries during power interruptions. They are the best solution for health facilities operating in the rural and semi-rural districts,” said Mulat Melese, MPH, vice-director of the Amhara Public Health Institute.
ICAP also trained laboratory personnel and clinical service providers on laboratory diagnosis and fever case management, respectively, providing mentorship and supportive supervision for quality assurance.
So far, 454 laboratory staff and 601 clinical service providers have received training through the current Malaria Diagnosis and Treatment Activity since it began in 2018. Combined with the 4,151 laboratory personnel and 4,193 clinicians trained during ICAP’s previous Malaria Laboratory Diagnosis and Monitoring project, ICAP has trained approximately 9,400 health care workers.
“Previously, we didn’t have high-tech laboratory equipment to support our diagnosis service and increase its level of accuracy; neither did we have the skilled workforce who could deliver quality services to the ever-increasing number of clients. This has been solved after ICAP supported us with in-service training and high-quality microscopes,” Alemtsehay stated.

Even the patient registers that log visits and services provided have been updated as part of the project: “We used to manually draw lines on plain paper to make registers,” Alemtsehay continued. “Now we are using a standard comprehensive laboratory register book supplied by ICAP.”
As the current project continues, ICAP is working to expand its support to 1,650 health centers, 3,300 health posts, 33 health science universities and colleges, eight biomedical equipment (BME) maintenance centers and over 100 BME maintenance workshops in Ethiopia to improve malaria diagnosis and case management.
“As the country has embarked on a new chapter in the fight against malaria that envisions realizing an end to malaria for good by 2030, ICAP’s continued support in the areas of malaria diagnosis and case management has been tremendously helping the effort toward elimination,” said Hiwot Solomon, BSc, MPH, acting director of disease prevention and control at the Ministry of Health.
ICAP’s work in Ethiopia began in 2005, focusing on support for the scale up of HIV prevention, care, and treatment for adults and children, and then evolving into a broad portfolio of technical assistance, capacity building, and transition support for HIV, tuberculosis, malaria, and other pressing health issues. Learn more on ICAP’s website.
A global health leader since 2003, ICAP was founded at Columbia University with one overarching goal: to improve the health of families and communities. Together with its partners—ministries of health, large multilaterals, health care providers, and patients—ICAP strives for a world where health is available to all. To date, ICAP has addressed major public health challenges and the needs of local health systems through 6,000 sites across more than 30 countries. For more information about ICAP, visit: icap.columbia.edu
Photo captions—Header image: A mother brings her infant to the Bure Health Center with an acute fever, and a health care worker takes a blood sample for laboratory microscopy for malaria diagnosis. Photo 2: A father and child at the Bure Health Center, one of 1,026 health facilities supported by ICAP through PMI. Photo 3: The Gambella region in Ethiopia, one of the high-burden areas prioritized by ICAP and PMI for rapid improvement in malaria diagnosis and treatment. Photo 4: A laboratory worker uses a microscope at the ICAP-supported Adama Hospital in Ethiopia.