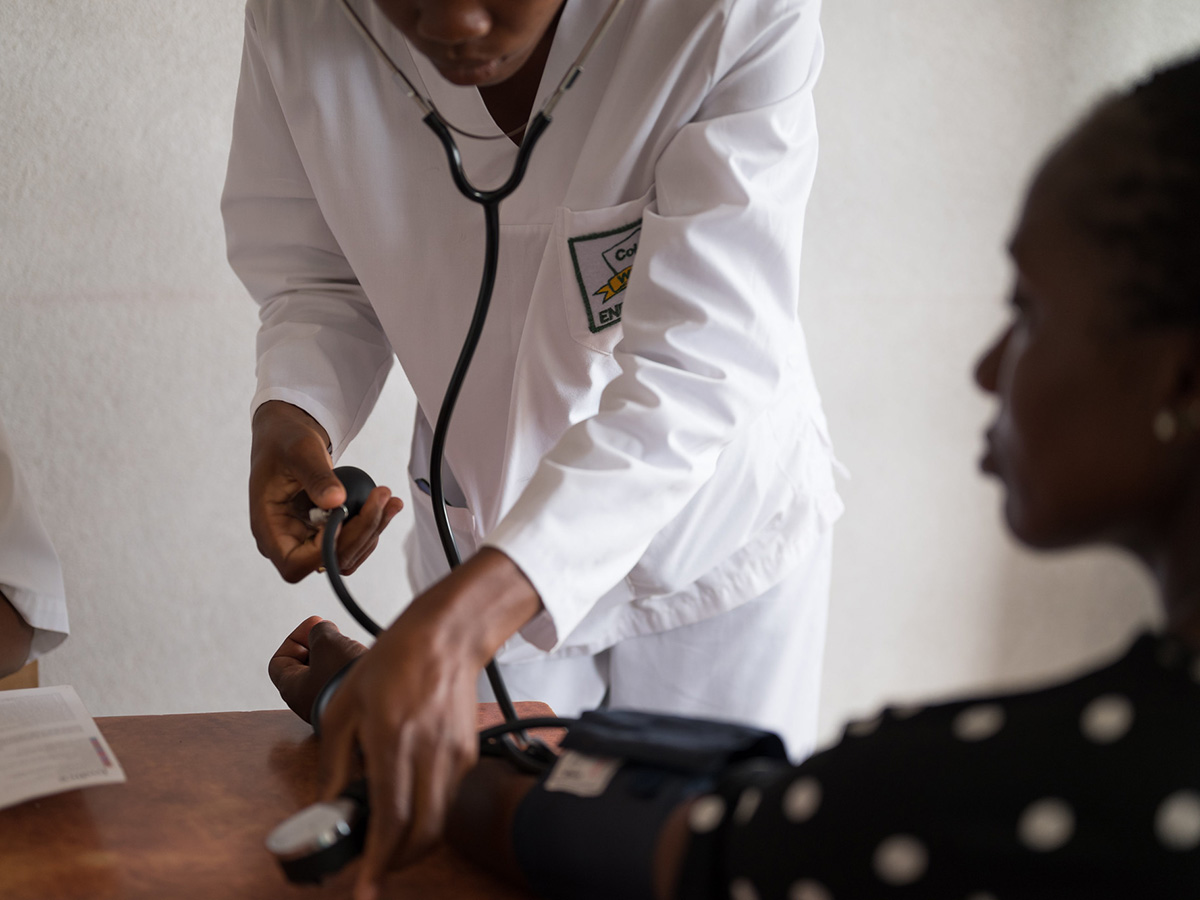
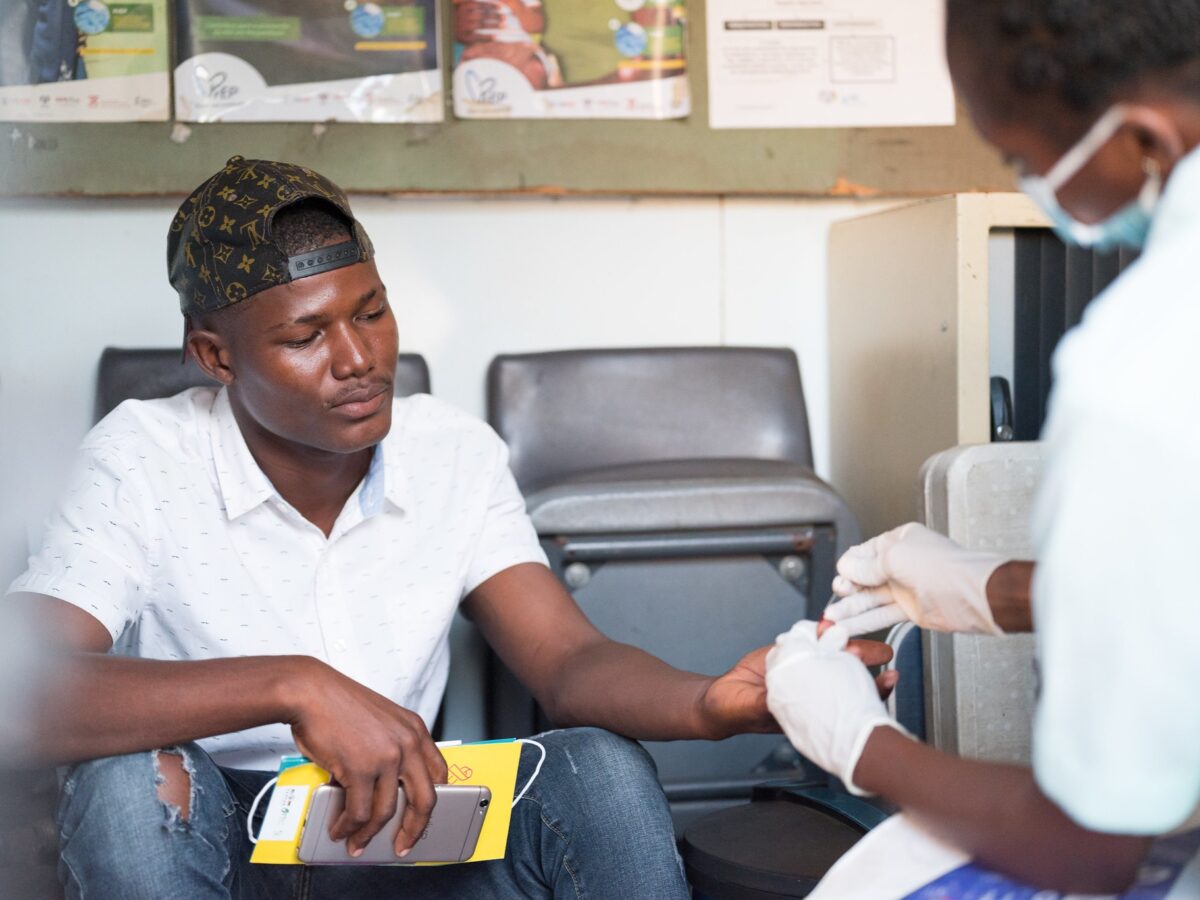
Members of a Community ART Refill Group (CARG) outside Harare, Zimbabwe, receive their medication in the community. CARGs help ensure people living with HIV get high quality HIVservices, stay healthy and receive social support.
At the turn of the 21st century, the global health community responded with new energy and focus to the HIV epidemic, which was claiming lives at an alarming rate in sub-Saharan Africa and around the world. Investments in prevention programs and access to antiretroviral therapy (ART) saved lives and slowed the spread of the virus. In the years since, demand for treatment has increased dramatically and people living with HIV(PLHIV) are accessing services in unprecedented numbers, overtasking busy providers and health facilities while resulting in undue burdens on the recipients of care.
Public health experts and international organizations have extolled the potential benefits of differentiated care, also known as differentiated service delivery (DSD), as a way to help health systems use resources more efficiently and better handle the demand for HIVservices. At the same time, with DSD, PLHIV whose disease is stable can access treatment and services, including social support, closer to home in their communities. Thus, they avoid long waits in crowded clinics and those living in rural settings can avoid frequent and costly trips to a health facility.
“The process is about putting people at the center of HIV services,” said Dr. Miriam Rabkin, director for Health Systems Strategies at ICAP and the principal investigator of the HIV Coverage, Quality, and Impact Network (CQUIN). “Programs can adapt and modify the intensity, frequency, provider type, and location of prevention and treatment services to adapt to the needs of people living with HIV. Ultimately, the goal is to improve the quality and coverage of HIV services as we move toward the UNAIDS 90-90-90 targets and epidemic control.”
While differentiated service delivery may appear straightforward, putting it into practice and scaling it up are inherently complex, and its novelty adds to that complexity. Implementing differentiated service delivery at the local and country level requires access to the right resources, multifaceted partnerships, and buy-in from ministries of health. Most importantly, it requires acceptance from the both patients and health care workers.
The CQUIN Learning Network for Differentiated Care
In 2016, ICAP embarked on a new three-year initiative to support countries in sub-Saharan Africa in scaling up differentiated service delivery from small pilot projects to large-scale national programs. Scale up requires expanding interventions or programs that serve a small proportion of the population to those that serve a significantly larger population (such as an entire region or country). CQUIN supports ministries of health as they share knowledge and tools to advance DSD, and facilitates joint learning about the science of scale-up. CQUIN partner countries have collaboratively prioritized focus areas (or “communities of practice”) based on their needs and contexts. The CQUIN project facilitates joint learning and co-creation of resources and tools to expand differentiated service delivery.
The vision is that by 2020, network country members will take differentiated services to scale, enabling more people living with HIV to initiate and sustain high-quality treatment, improving individual health and achieving population-level impact.
July was a busy month for CQUIN. It held its first “community of practice” workshop, focused on differentiated service delivery for patients at high risk of HIV disease progression. The three-day gathering held from July 17-19 in Harare, Zimbabwe, brought together nearly 70 participants from the nine network member countries: Ethiopia, Kenya, Malawi, Mozambique, South Africa, Swaziland, Uganda, Zambia, and Zimbabwe.
Persons living with HIV at high risk of disease progression include those with advanced disease at the time of diagnosis, as well as those who have been on antiretroviral treatment for a year or more but have an unsuppressed viral load, or have other issues requiring close follow-up. Members of CQUIN network countries identified this topic as a priority community of practice at the CQUIN launch meeting in March 2017. The topics of the presentations in Harare ranged from innovative research to perspectives of people living with HIV and considerations for policymakers and implementers working to scale up differentiated care.

CQUIN at IAS 2017
On the heels of the CQUIN workshop in Harare, ICAP organized a satellite session at the International AIDS Society’s annual conference (IAS 2017) in Paris on Sunday, July 23. The session – Differentiated Service Delivery: Innovating for Impact – included an interactive panel discussion that focused on the latest innovations identified by the network. Dr. Bactrin Killingo, treatment and education lead at the International Treatment and Preparedness Coalition (ITPC) and Dr. Tsitsi Apollo, deputy director for HIV/AIDS and STIs at the Zimbabwe Ministry of Health (pictured right, above) moderated the session, with presenters from the Ministries of Health of Zimbabwe, Mozambique, and Swaziland, as well as civil society and implementing partners.
Dr. Wafaa El-Sadr, ICAP’s global director, opened the session with framing remarks emphasizing the important role that coverage, quality, and efficiency – all cornerstones of the CQUIN network – play in reaching the 90-90-90 targets, while Dr. Peter Preko, CQUIN project director, provided an overview of the Network. Dr. Aleny Couto, head of the National HIV/AIDS Program at Mozambique’s Ministry of Health, discussed that country’s community ART groups, while Dr. Nomthandazo Lukehle, national ARTcoordinator in Swaziland, described the challenges associated with designing differentiated care models for patients with both HIV and non-communicable diseases. Dr. Maureen Syowai, regional technical advisor for ICAP in Kenya, recapped the Harare workshop and highlighted issues related to differentiated service delivery for patients at high risk of disease progression, and Dr. Bill Reidy, strategic information specialist at ICAP, summarized key issues and challenges related to monitoring and evaluation (M&E) of DSD. All of the presentations are available on the IAS 2017 website. Dr. George Ayala, executive director for the Global Forum on MSM, made the concluding remarks by addressing the challenges for scaling up differentiated service delivery for key populations.
The next steps for CQUIN include launching additional communities of practice, including those addressing DSD for adolescents and the monitoring and evaluation of DSD. Additional in-person workshops and online learning platforms are planned as ICAPcontinues to facilitate joint learning and sharing of valuable resources among network members.
“If done right and done together with communities and other stakeholders, differentiated service delivery can be a tool to achieve excellence at scale, and improve the health and well-being of the populations we all care about,” said Dr. Peter Preko, CQUIN’s Project Director. “ICAP and CQUIN are enabling countries to share experiences, innovations, and best practices so they can move differentiated care from pilot projects to national programs.”
Receive updates on CQUIN and the latest news and resources on differentiated care by signing up for the network’s monthly newsletter.