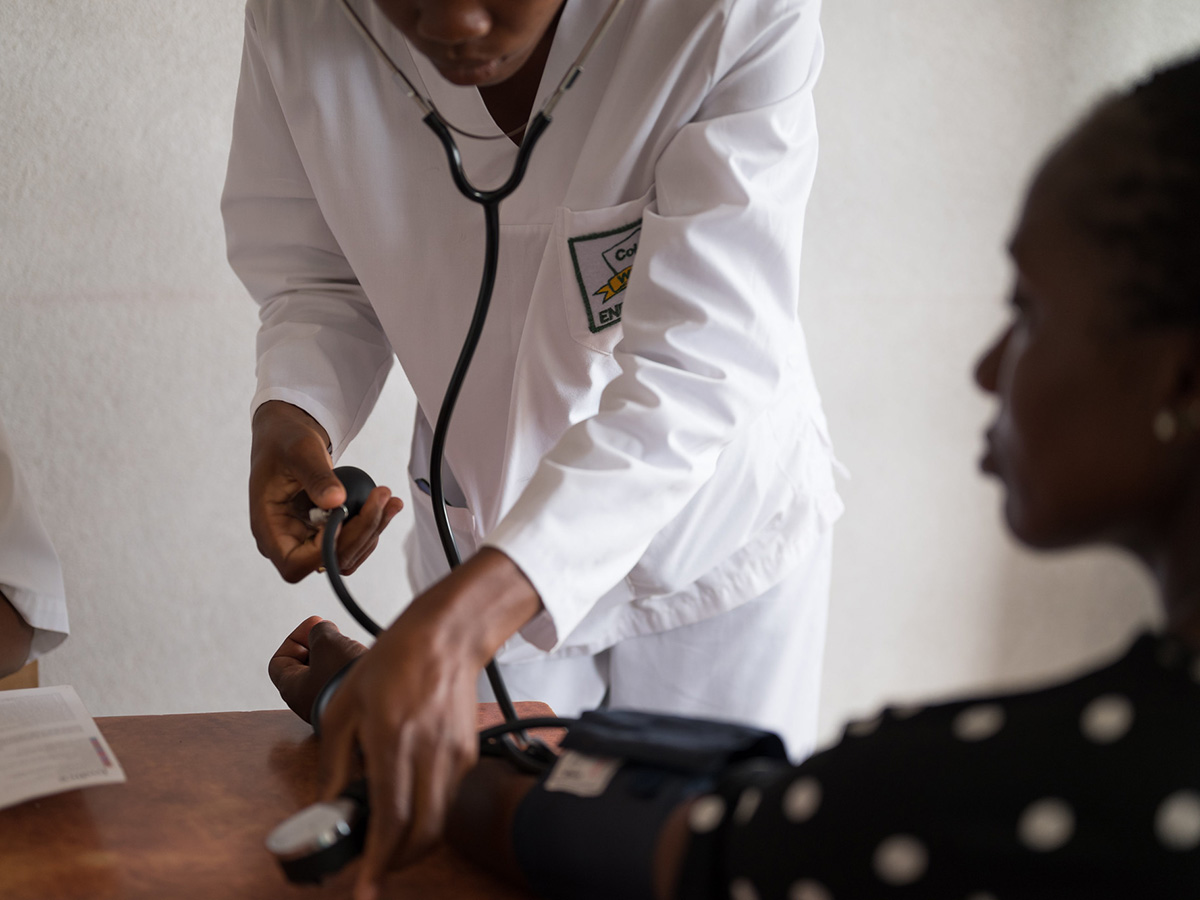
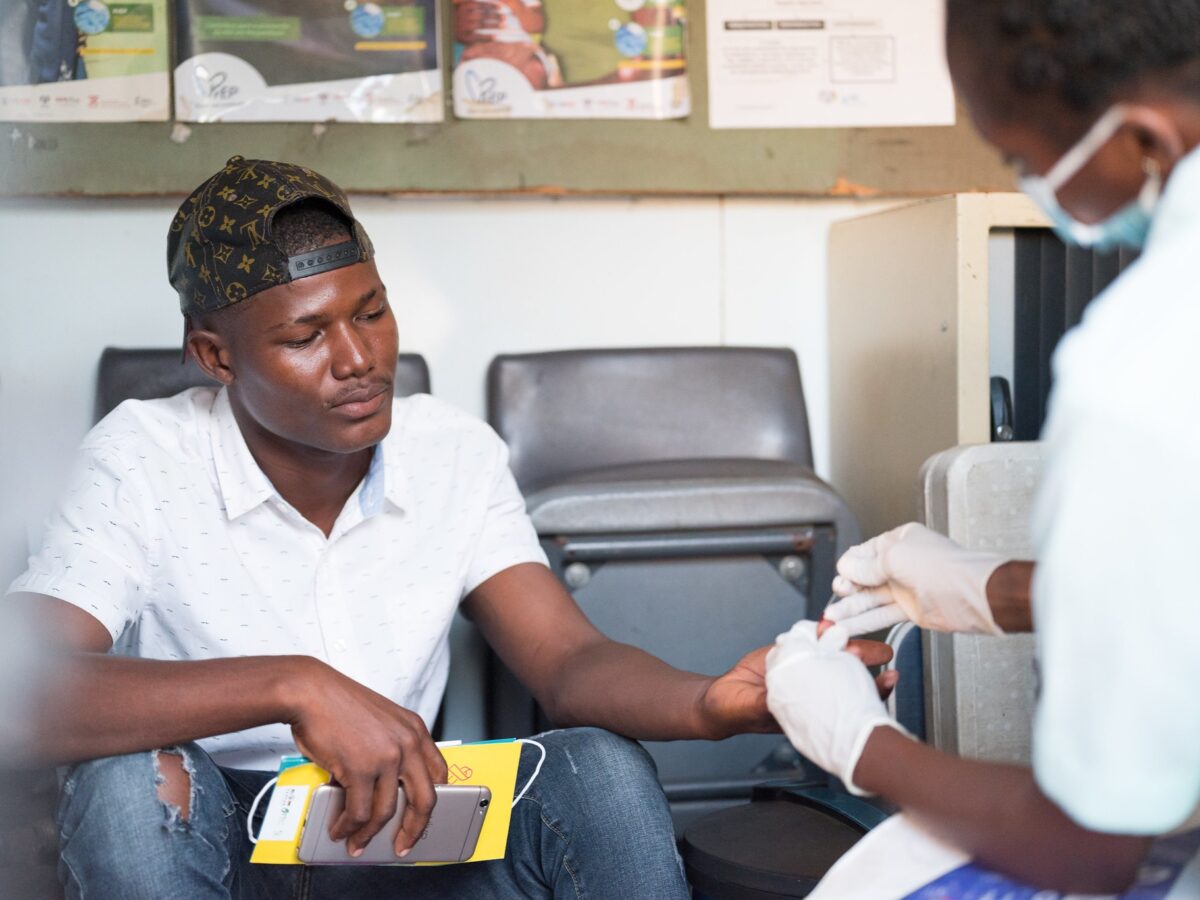
Eswatini has one of the world’s highest rates of new tuberculosis (TB) cases. Children in particular are extremely vulnerable to severe forms of TB disease. In 2018, over one million children developed TB globally, and at least 7.5 million children are estimated to have been exposed to the infectious disease at the household level.
To develop interventions and improve TB prevention in children, ICAP at Columbia University is leading a study in Eswatini that customizes child TB contact management (CCM) for children exposed to TB in the household.
CCM – which requires identifying and screening child contacts exposed to adults with TB and ensuring initiation and completion of either TB preventive treatment (TPT) or TB treatment – has long been recognized as an important method for addressing childhood TB. However, stigma and access to care, hinder CCM from seamlessly ensuring rapid identification, screening, and initiation and completion of appropriate treatment for child contacts.
ICAP’s Flexible InteRvention Strategy for TB prevention (FIRST) study is pilot-testing a person-centered CCM model in which families choose whether they would like their children to receive facility- or community-based TB prevention services. The study, assessing the feasibility and acceptability of the intervention strategy, is being delivered in the Manzini region of Eswatini with the premise: “one size does not fit all.”
“Conventional CCM models can be binary,” said Yael Hirsch-Moverman, PhD, MPH, assistant professor of epidemiology at Columbia University and lead researcher of the ICAP study, “but we know that every family’s and child’s needs, concerns, and conditions are unique. A mother who has several children may not be able to travel to a healthcare facility to get her child access to TB screening, for example, while another family may not want to risk health care workers visiting their home for fear of stigmatization. All these factors go into a family’s decision as to how they want to address TB in their household.”
Traditionally, TB patients have limited participation in their care in high burden settings and seldom inform the planning and development of health care services or one-on-one patient-provider consultations. FIRST involves formative research with caregivers of child contacts – as well as with healthcare providers who deliver services – to understand when and how TB prevention services should be delivered to best meet each family’s needs. A stakeholder working group assists in incorporating feedback from the research to refine the intervention strategy.
FIRST builds on past ICAP studies, including the PRovide Options for Treatment of Exposed Children against TB (PROTECT) study, which examined preferences among HIV-positive children, caregivers, and health care providers regarding TB preventive treatment regimens and service delivery models offered to child contacts. PROTECT found that palatable medication, smaller and fewer pills, low visit costs, and shorter clinic wait times are important factors when designing TB prevention services for children. FIRST also builds off the ICAP-led PREVENT study, which found that barriers to successful CCM for young children vary from family to family, even within the same community. The study showed that caregivers of child contacts were interested in being involved in their children’s treatment decisions.
“The World Health Organization roadmap for childhood TB recommends a ‘family and community-centered strategy’, but there are limited formal evaluations of interventions that address barriers to a seamless CCM program,” added Hirsch-Moverman. “Interventions to address TB and other chronic health issues must be responsive to the needs, conditions, and access to resources of individual communities and families to be successful both in the short- and long-term.”
For the first time in over a decade, TB-related deaths increased in 2020. As World Tuberculosis Day approaches on March 24, with this year’s theme Invest to End TB. Save Lives, it is more critical than ever to ensure equitable access to preventive TB resources to decrease the incidence of the disease.
Only 4 percent of reported TB cases in Eswatini are in children, which is much lower than in similar settings, reflecting substantial underdiagnosis of the disease. Given that Eswatini also has the highest rate of HIV prevalence in the world, effective CCM could have substantial implications within the country.
“FIRST can help provide policymakers, clinicians, and researchers with robust data and a rigorous framework to inform the improvement of CCM in high TB and HIV burden settings,” said Andrea Howard, MD, MS, director of ICAP’s clinical and training unit and a collaborator on the study. “This study will help us to continue to refine a flexible intervention strategy for CCM so that in the future we can evaluate the effectiveness, cost-effectiveness, and feasibility of such measures on an even larger scale.”
About ICAP
A major global health organization that has been improving public health in countries around the world for nearly two decades, ICAP works to transform the health of populations through innovation, science, and global collaboration. Based at Columbia Mailman School of Public Health, ICAP has projects in more than 30 countries, working side-by-side with ministries of health and local governmental, non-governmental, academic, and community partners to confront some of the world’s greatest health challenges. Through evidence-informed programs, meaningful research, tailored technical assistance, effective training and education programs, and rigorous surveillance to measure and evaluate the impact of public health interventions, ICAP aims to realize a global vision of healthy people, empowered communities, and thriving societies. Online at icap.columbia.edu