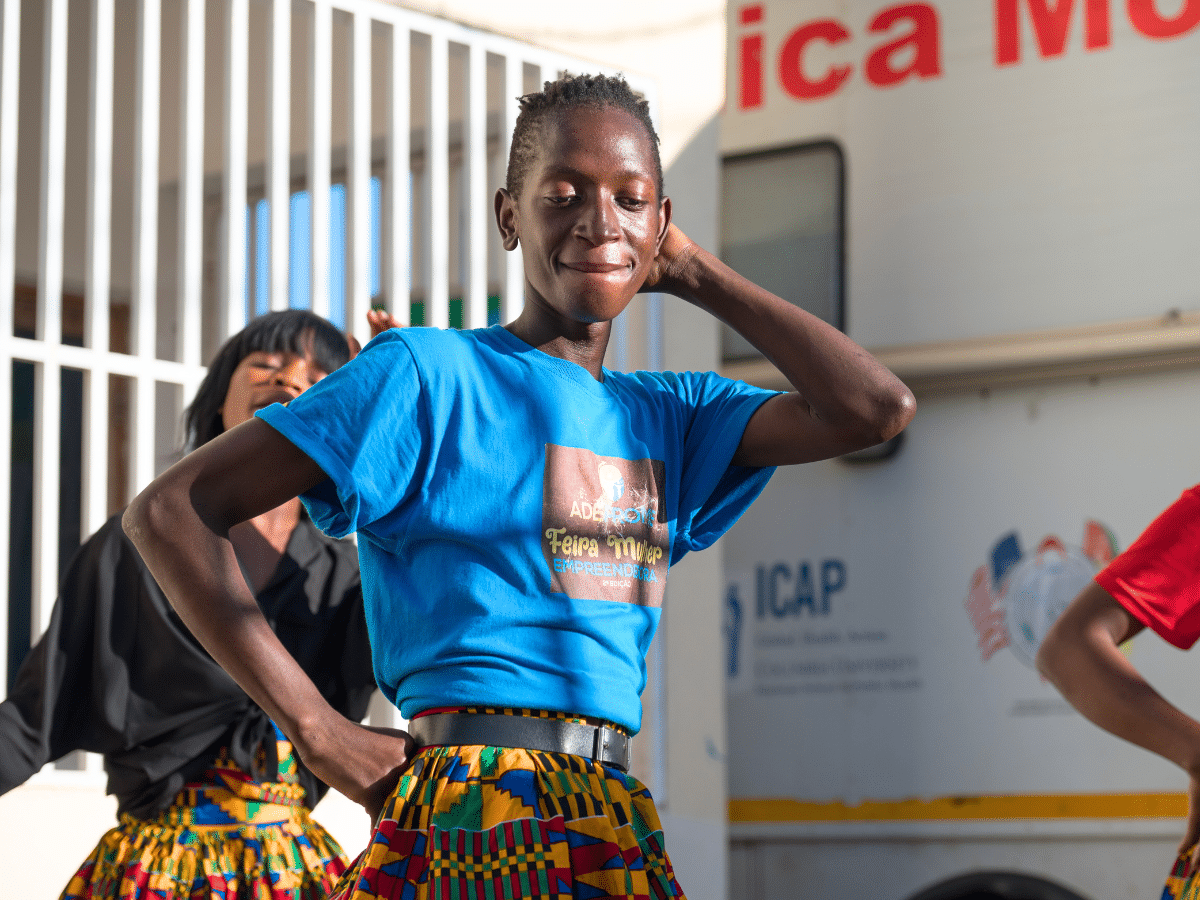During his first week at a hospital in Maputo, Mozambique, Albano,* a first-year health management student, was all nerves. One day he noticed there were no barriers between dirty and clean laundry areas, and laundry workers passed freely between the two, resulting in cross contamination. He scribbled some notes in his pad, took a deep breath, and walked to share his concerns with his instructor and hospital staff.
“Being the new person is intimidating,” he said. “Especially when part of my job is to point out what isn’t working.”
Albano is one of 50 students assigned to hospitals across Maputo to complete a series of on-site rotations as part of the new four-year bachelor’s degree program in health management and administration at the Instituto Superior de Ciências de Saúde (ISCISA). While most of the students have only recently finished high school, their practica placements could represent a sea change in hospital management in Mozambique, where despite a severe shortage of physicians, doctors often work as administrators instead of focusing directly on patient care.
The health management administration degree program is the result of a partnership between ICAP, Mozambique’s Ministry of Health, ISCISA, and the Department of Health Policy and Management at Columbia’s Mailman School of Public Health. Funded by USAID, the project has remodeled ISCISA’s curriculum to create a degree program that produces graduates whose skills are more aligned with Mozambique’s national health needs.
According to Professor Paul Thurman of the Mailman School, learning to manage health facilities is a key factor in the fight against major health threats such as HIV, because it makes health systems stronger and more efficient. “If you free up doctors’ time that’s a good thing,” he said. Professor Thurman leads the project, along with Dr. Miriam Rabkin, ICAP’s director for health systems strategies.
“If the goal is to improve health services, you have to improve some very basic systems and infrastructure as well. Otherwise it doesn’t matter how much surveillance and information we have,” Thurman explains.
Central to the new 37-course curriculum are ongoing practica where students work directly in hospitals to receive hands-on experience and the opportunity to develop solutions to real life challenges. There are eight practica, covering a range of topics from financial management to work scheduling. Albano is currently enrolled in the infection prevention and control practica, which has emerged as an especially important course.
Infection prevention and control is one of the cornerstones of an effective hospital. In addition to providing effective care and treatment, health facilities must put in place measures to protect staff and patients from hospital-acquired infections and other hazards. In developed countries, hospital acquired infections affect between three and 12 percent of patients, but in sub-Saharan Africa, the World Health Organization estimates this number to be significantly higher.
In Mozambique, where some health facilities lack soap and running water and infectious waste is often disposed improperly, patients are particularly at risk. Thus, while Albano was nervous about reporting his discovery to senior medical staff, it’s exactly what the developers of the program hoped for.
“It proves practica are working and that’s what we hoped for,” says Christopher Pupp, ICAP’s project director and curriculum design specialist, who was pleased to learn that a first year student is actively working with staff to fix such a major issue.
“Before the new curriculum, health management students didn’t begin practicing in hospitals until their final year,” he says. “Now students are placed directly in facilities from the outset of the program, which allows them to experience challenges and troubleshoot solutions on location from the very beginning.”
In addition to completing rigorous coursework, students learn about specific sanitation needs, such as how to manage temporary interruptions of water supply in hospitals and how to avoid cross contamination when laundry facilities are limited. Even though many students have only completed two of the eight practica, some are already showing they have to chops to manage and administer hospitals.
“These students really understand hospital waste management and they showed us a lot of mistakes we are making,” said a leading instructor at one of the placement hospitals. “It was actually a health administration student who pointed out we needed to use separate rooms for washing dirty laundry and ironing clean laundry.”
Students also recommended the use of specialized face masks for admissions staff working in the respiratory hospital where large numbers of tuberculosis patients receive care. Others detailed areas where hospitals were mixing infectious and noninfectious waste, lacked soap in patient bathrooms, and had inadequate cleaning schedules.
While the previous health management curriculum trained students based on ideal hospital conditions with modern equipment and fully-stocked infirmaries, this one is centered on Mozambique’s specific health challenges. Students no longer spend hours on coursework with no exposure to the real context. And that’s a good thing.
With this new training, Albano and his classmates won’t be nervous for long. Instead, over the course of four years, they will become part of hospital staff working to create safe and efficient systems, while freeing clinicians to provide essential health care.
That’s just the way it should be.
*Not his real name.