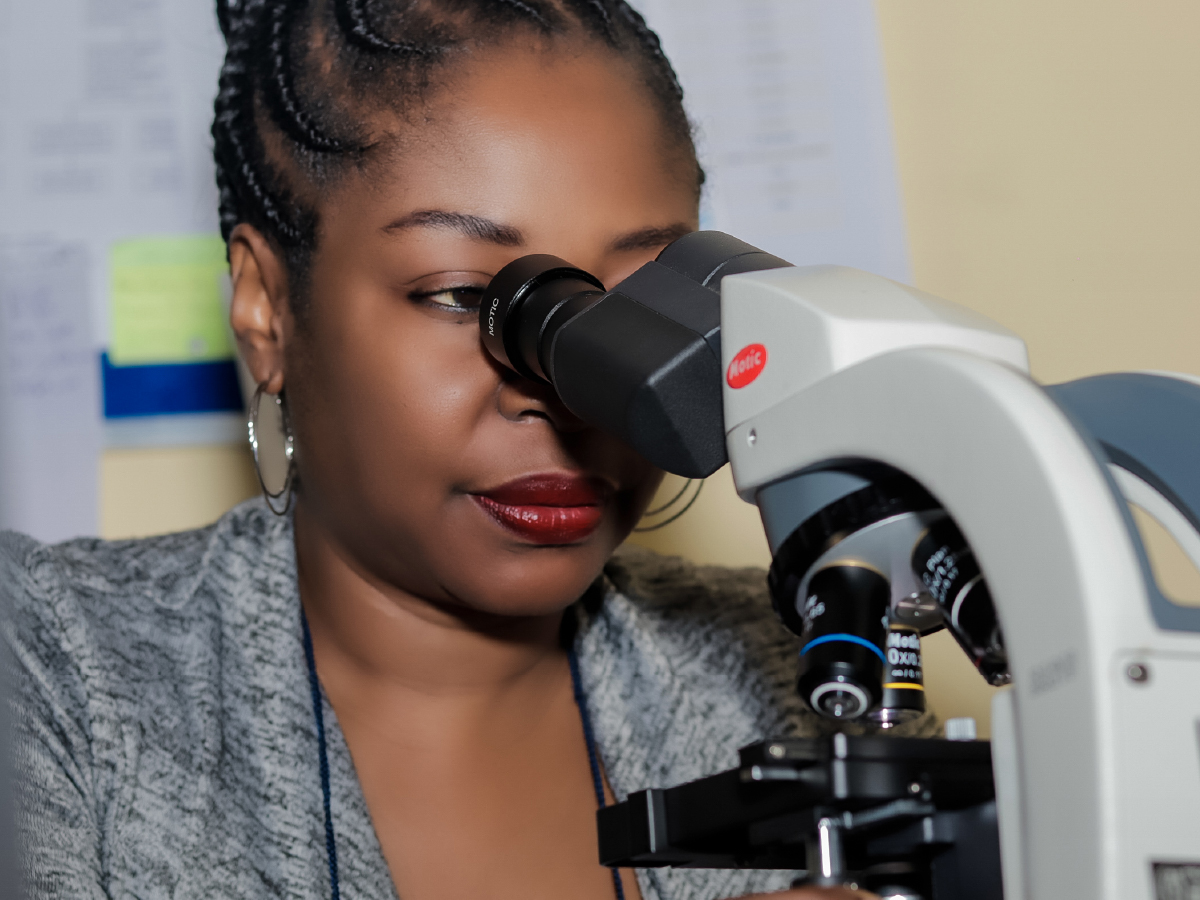
As a teenager growing up in Nigeria, ICAP’s Ima-Abasi Bassey was a voracious reader of romance novels, finding an escape in an ongoing series detailing dramatic tales of love among health professionals. This was a world where anything could happen and the stakes were high. The doctors in her stories stared into the eyes of death itself, confronting profound suffering, betrayal, and loss. In this world, doctors balanced life and love—and all the while, they pieced together symptoms, medical histories, and other clues to solve difficult medical cases and, ultimately, provide their patients with hope.
Never one to back down from a challenge or to follow a traditional path, Bassey set out to find a niche within the medical field, inspired by the characters in her favorite novels. While studying for her medical degree, Bassey had completed a number of rotations in pathology—the branch of medicine that deals with the laboratory examination of samples of body tissue for diagnostic and forensic purposes—but at the time, the field had not yet sparked her interest. Then, during her housemanship— a compulsory one-year program that medical professionals in Nigeria are expected to undergo after graduating from medical school—Bassey found herself drawn to the field. Following the encouragement of a mentor who was a pathologist working at her assigned hospital, she decided to pursue pathology as her field of practice and has never looked back.
Bassey works as ICAP’s lead pathologist on the Child Health and Mortality Prevention Surveillance (CHAMPS) project in Sierra Leone, a multi-year initiative led by Crown Agents and supported by ICAP, where she leads a team of specialists working together to reduce mortality by building knowledge through the collection accurate, timely, and reliable data on the causes of death and sickness in young children. The project uses an innovative alternative to traditional autopsy known as minimally invasive tissue sampling, or MITS. The technique, which involves the collection of tissue samples with core needles, allows researchers to quickly identify the cause of death, and help illuminate ways to save lives and improve the health of children in these vulnerable areas. In her role, Bassey chairs a panel of specialists from various medical fields who weave together data compiled through qualitative interviews with affected families and communities, as well as tissue samples gathered through the MITS procedure.
For Bassey, each collected sample is an important part of a story with the power to save lives. Once her team establishes cause of death, findings are shared with families, community groups, and public health officials to drive health interventions, research, and action to save young lives. As Sierra Leone continues to recover from the deadly 2014 Ebola epidemic, the country’s health system is fighting against numerous pervasive challenges, including extreme poverty, lack of clean water and sanitation infrastructure, poor nutrition, and maternal mortality rates six times higher than the global average. In this context, knowing how and why young children are dying is a critical first step towards creating solutions to give children a fighting chance at survival. Her team’s analysis provides decision makers at local, district, and national levels with a full picture of each child’s death, ensuring that, in the wake of such a tragedy, preventative measures are in place to make an immediate impact and safeguard the lives of others.
While fiction was her inspiration, Bassey has long been steeled to the tough reality of the work she does. “You never get used to people dying,” she said. “But, if there is no lab work, there are no answers.”